Poster Presentation Annual Meetings of the Endocrine Society of Australia and Society for Reproductive Biology and Australia and New Zealand Bone and Mineral Society 2016
Impact of substantial weight loss on thyroid function in obese women planning pregnancy (#391)
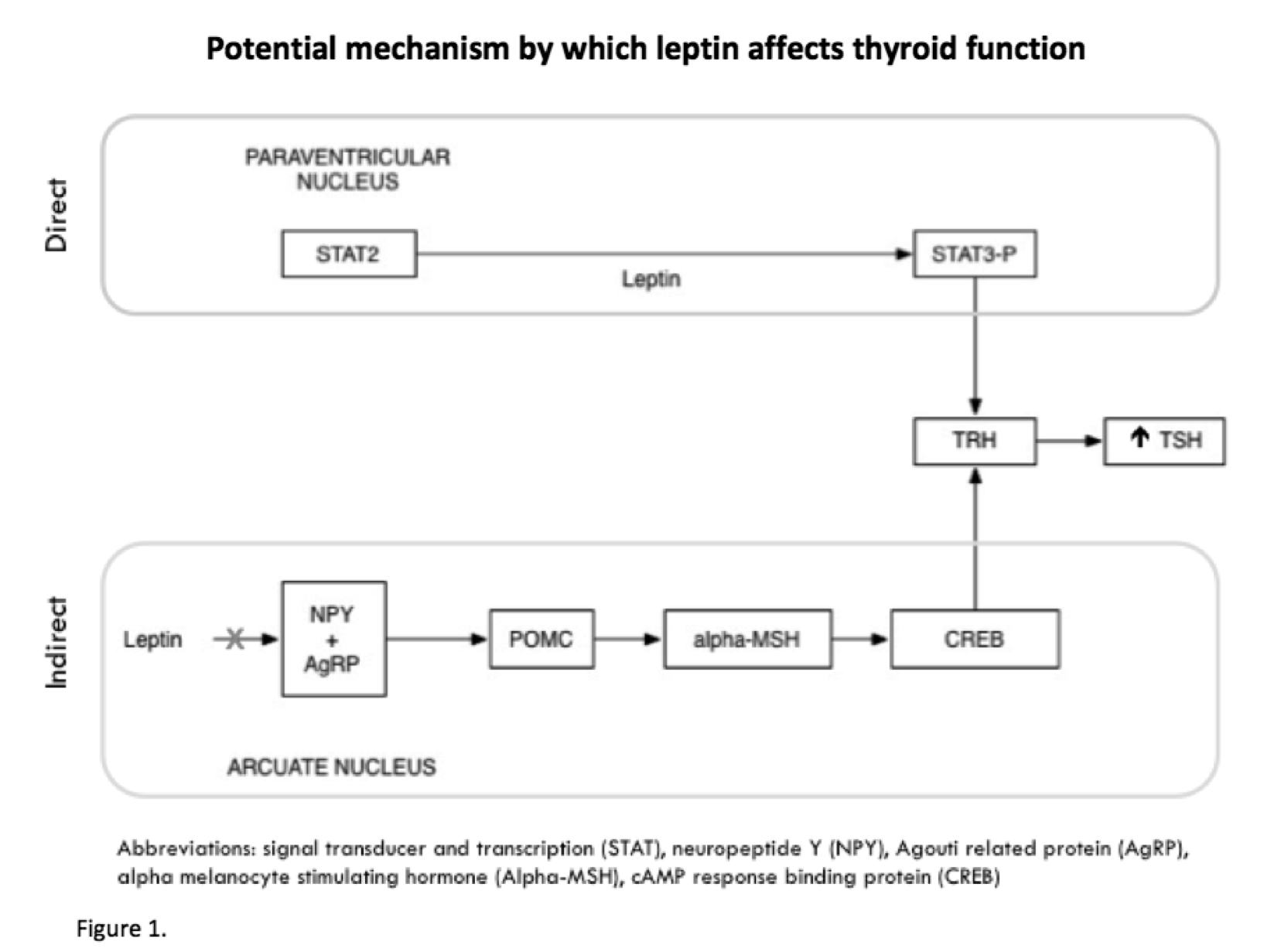
Background: Maternal obesity is associated with significant maternal and neonatal complications. To address this, weight-loss must begin pre-conception. Hypothetically, substantial weight-loss could be accompanied by changes in thyroid function (figure 1). Given thyroid hormones are crucial for early fetal neurodevelopment, it is imperative to understand these changes. The impact of both modest and substantial weight-loss on thyroid function have been poorly described. Furthermore, there are no prospective studies evaluating the effects of weight-loss on thyroid hormones in the context of pre-pregnancy care.
Objective: To investigate the impact of substantial weight-loss on thyroid function in obese women planning pregnancy.
Method: Obese pre-pregnant women aged 18-38 years were randomised to substantial weight-loss (VLED diet) or modest weight-loss (lifestyle advice based on current Australian guidelines) for 12 weeks. Fasting blood samples were collected at baseline and 12 weeks for measurement of thyroid function (fT3, fT4 and TSH). In a subset of 11 women who fell pregnant after the intervention, a third blood sample was collected at 12 weeks gestation for analysis. All samples from the pregnant subgroup were further tested for rT3 levels.
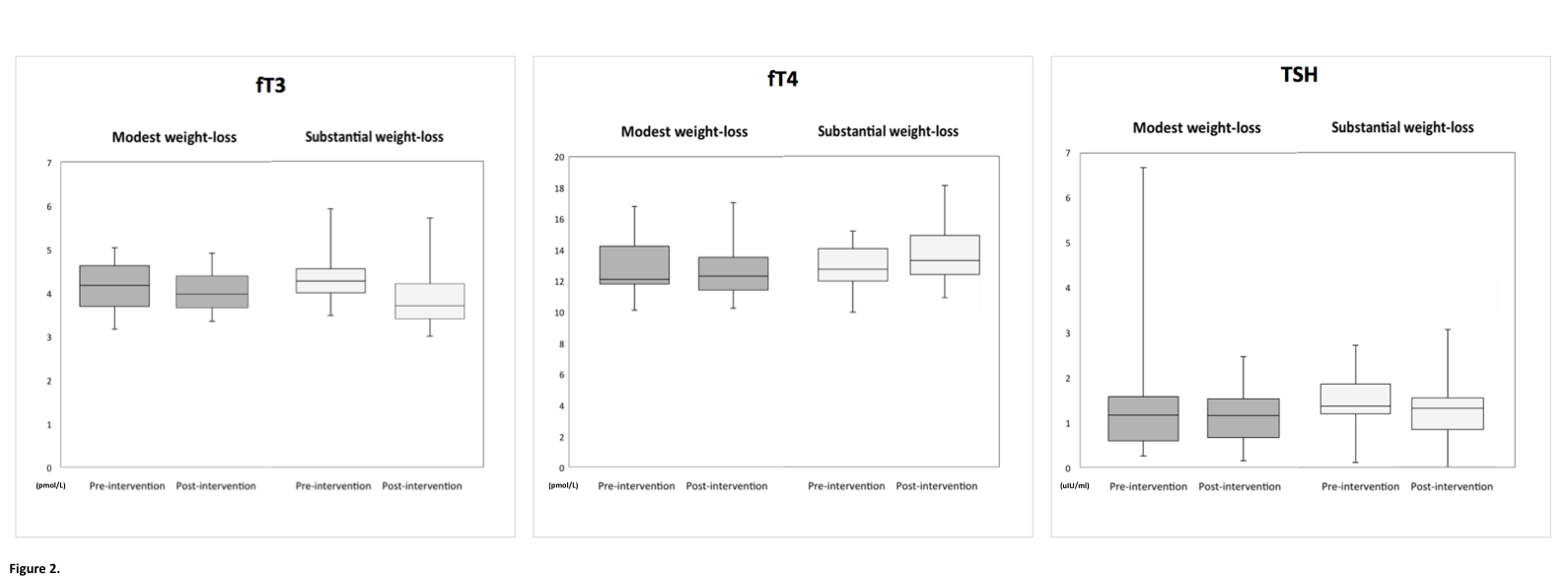
Results: 48 women (mean age: 33.78±3.28, mean parity: 0.75±1.13, mean BMI: 36.84±6.36kg/m2 and mean weight 98.94±18.67kg) were randomised as above. Total body weight-loss in the substantial and modest weight-loss arms were 13.87±4.22kg and 2.55±2.03kg respectively. There were no statistically significant differences in the levels of serum fT3, fT4 or TSH between those with modest weight-loss and those with substantial weight-loss at baseline, week 0 and 12 weeks gestation (figure 2).
Conclusions: Substantial preconception weight-loss is not associated with statistically significant changes in serum levels of fT3, fT4, TSH or rT3 prior to pregnancy or in early pregnancy when compared with women who achieved modest weight-loss. Reassuringly, pre-pregnancy weight-loss does not significantly alter maternal thyroid function.